Acute and chronic hives and rashes and their causes and treatments can be tricky. There are many different conditions that can cause bumps, rashes, or itchy skin. In many cases, the conditions are temporary and quickly disappear with treatment. In other cases, hives or rashes can last long-term and are more difficult to manage. Your primary care physician or a dermatologist can help diagnose skin conditions and recommend a proper treatment plan. (For more on dermatological issues, see my article on how to treat skin conditions; eczema, seborrhea and psoriasis.)
Acute vs. Chronic
When diagnosing and treating skin problems, it helps to know whether the condition is acute or chronic. Acute conditions appear quickly and often within a few days. The skin’s appearance may change within a day or two, overnight, or even within a few minutes. Symptoms may also get worse fast.
On the other hand, chronic conditions are present for several weeks or longer and they may tend to worsen over a longer time period. Chronic conditions may appear on their own or may develop as a result of acute skin conditions that go untreated.
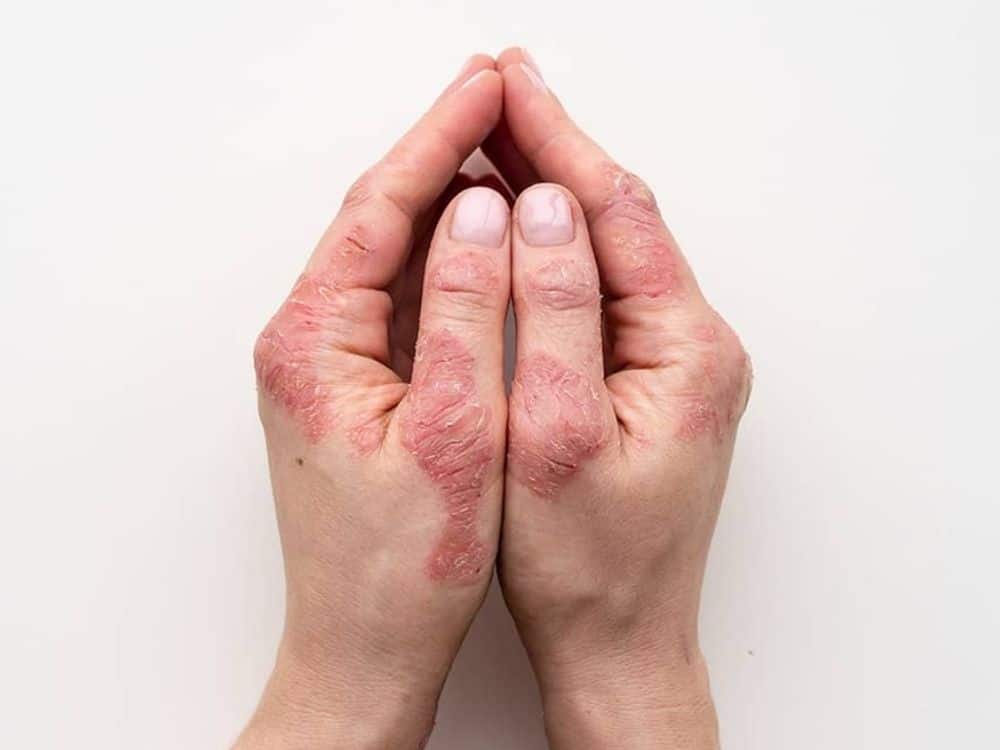
What Are Hives?
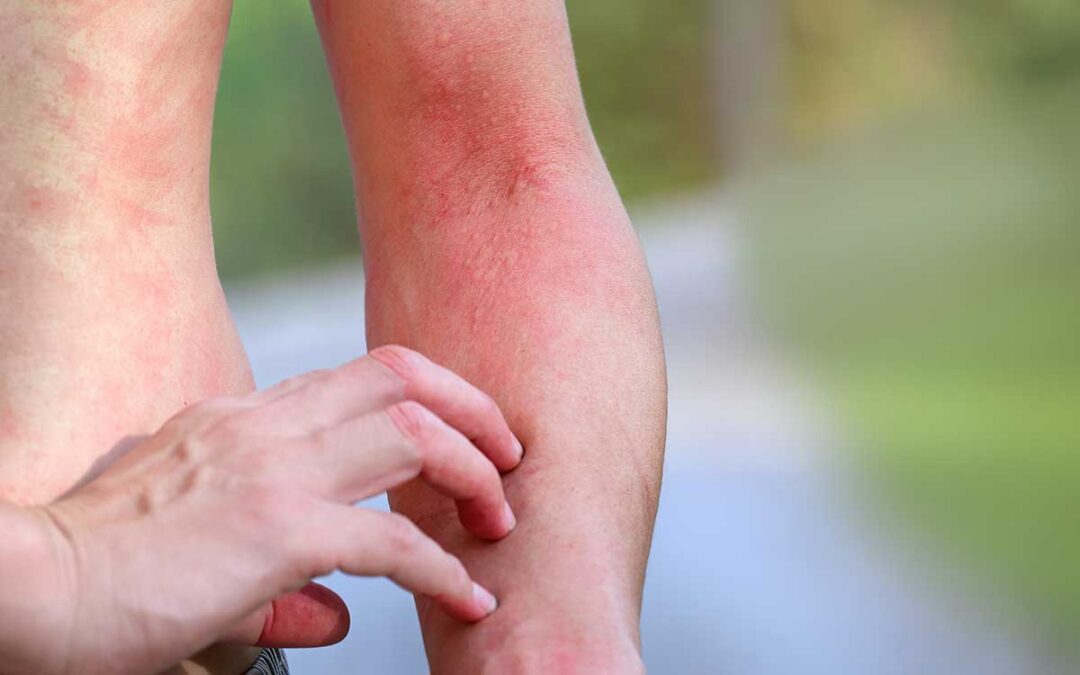
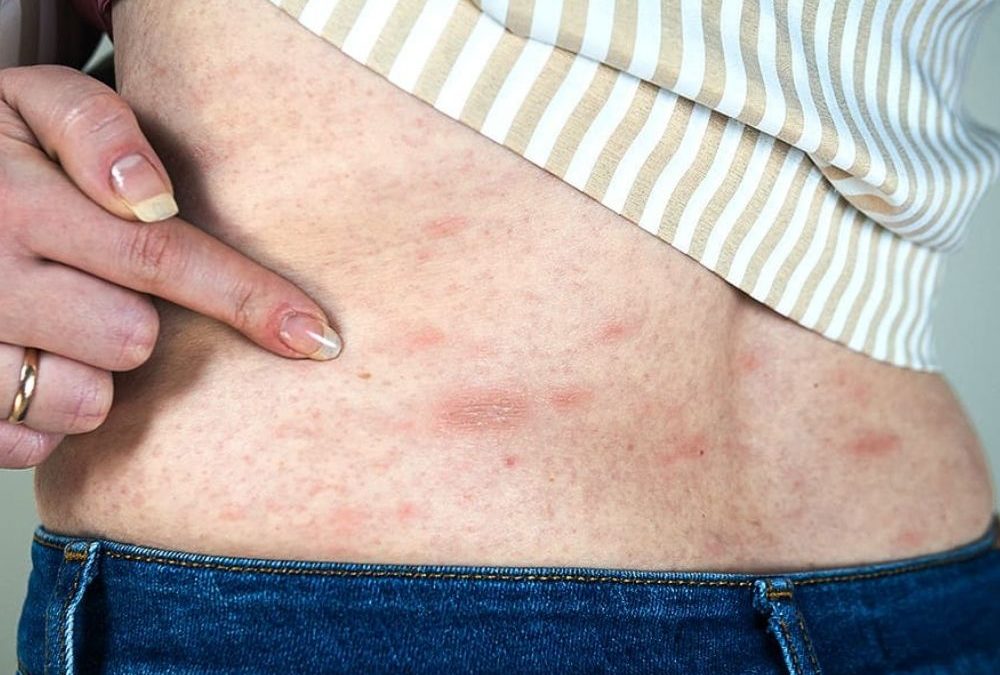
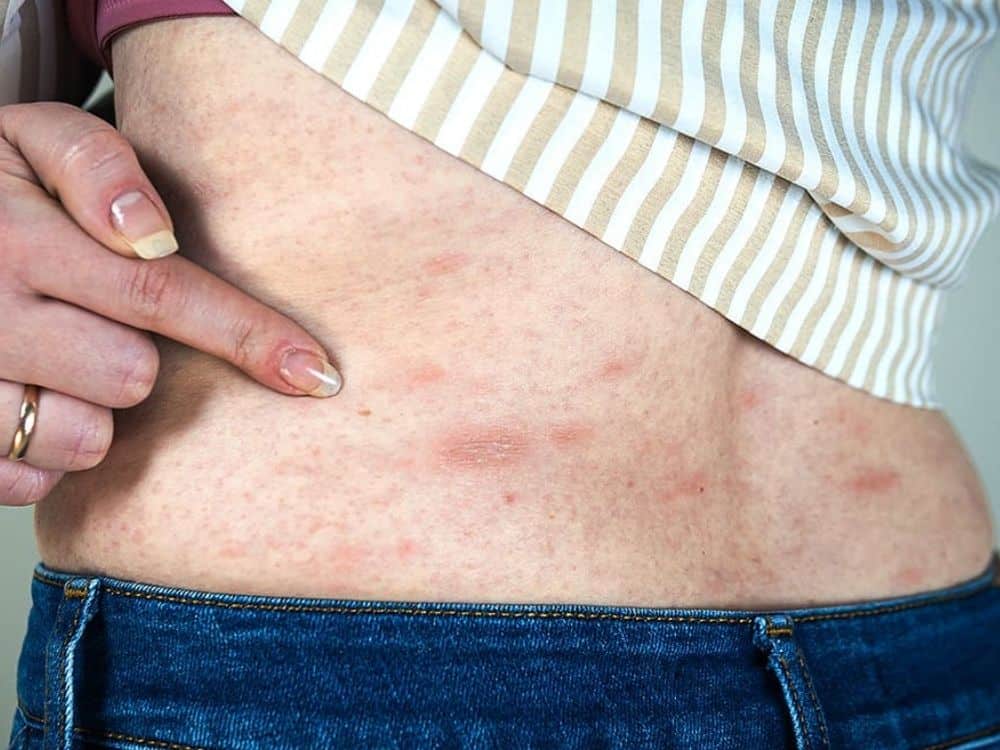
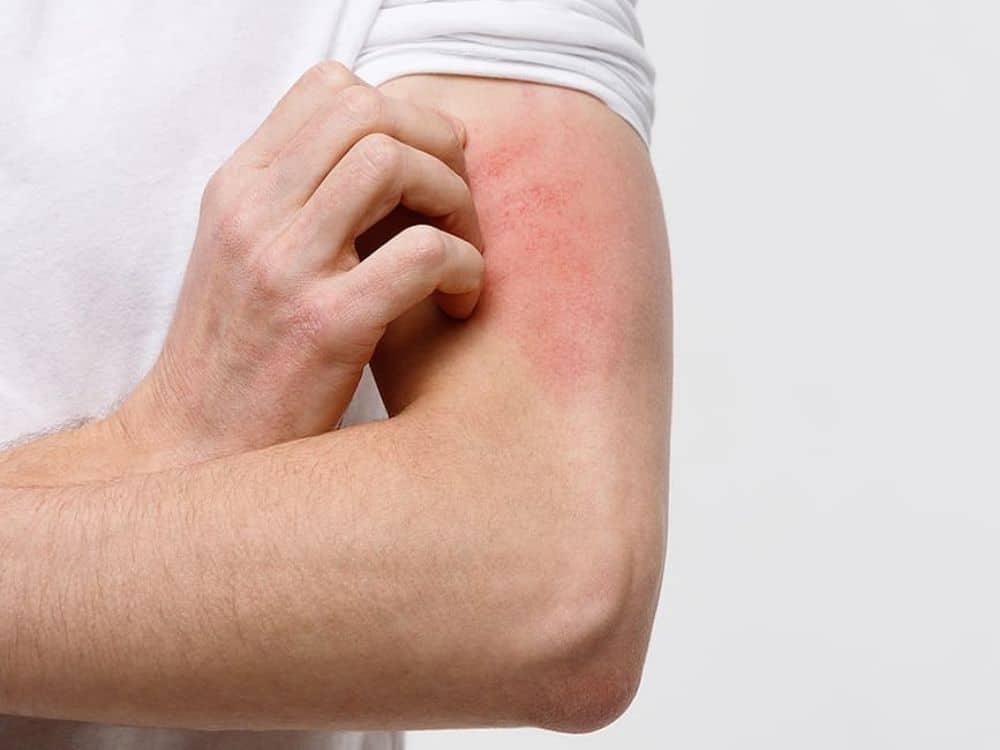
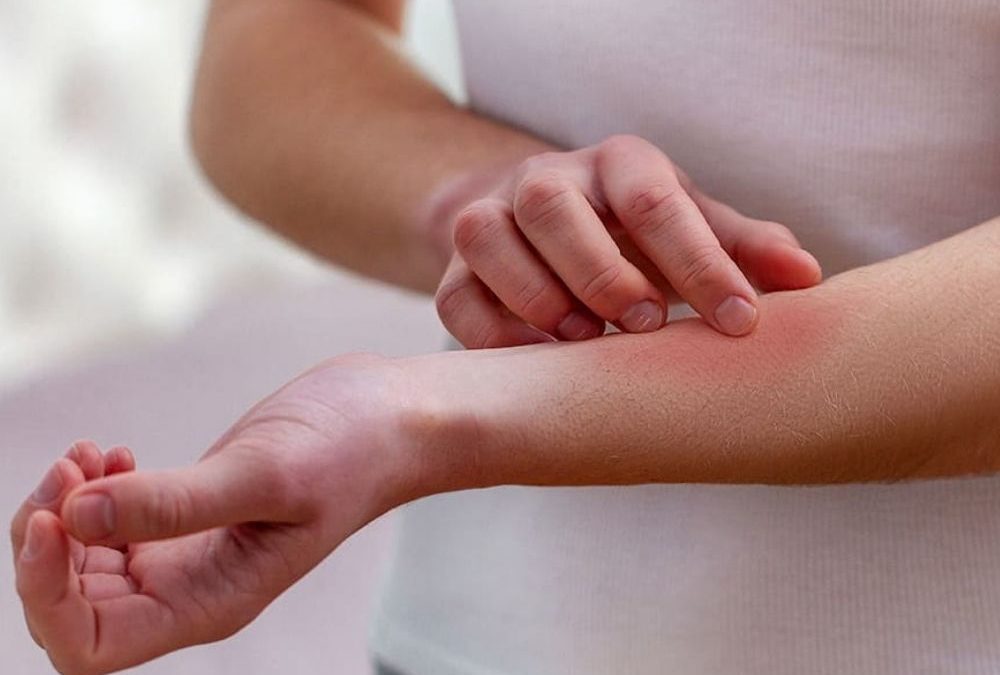
Hives are bumps that stick out from the skin. These bumps, also called urticaria or wheals, are itchy and usually appear red in color, although this redness can be harder to see on darker skin colors. Hives may also appear as flat, raised patches on the skin. The bumps and patches may grow larger, change shape, or go away over a short time period. Hives are common, affecting up to 1 in 5 people at some point in their lifetime.
Hives are usually caused by an allergic reaction. When a person comes in contact with something they are allergic to, the immune system creates inflammation, which may lead to hives and swelling. Things that may create an allergic response and lead to hives include:
- Pollen, mold, or dust
- Bug bites
- Animals, including cats or dogs
- Foods, including nuts, dairy products, eggs, meat, or seafood
- Chemicals such as latex
- Certain soaps, detergents, or cosmetic products
- Medications such as aspirin, penicillin, vitamins, birth control pills, and non-steroidal anti-inflammatory drugs (NSAIDs)
Hives aren’t always an allergic reaction. Sometimes, they form when a person is feeling stressed, sweats a lot, exercises, or has been in very hot or very cold temperatures. Infections like mononucleosis (mono), sinus infections, tooth infections, or COVID-19 can also lead to hives. Another possible cause is diseases like lupus, thyroid disorders, or lymphoma. In some cases, doctors don’t know what has caused a particular case of hives.
Hives can be acute or chronic. Acute hives usually appear and disappear within a period of hours or days. They may come back over the next couple of weeks, but will usually go away again quickly. Chronic hives continue to reappear, sometimes multiple times per week, over a period of 6 weeks or more.
Treating Acute Hives
Acute hives often disappear without any treatment. To help the skin recover, you can avoid hot water and tight-fitting clothing. Antihistamine (anti-allergy) medication can help calm these allergic reactions. Severe hives may need to be treated with stronger medication or a shot.
Allergens can sometimes cause a severe allergic response called anaphylaxis. You may need emergency medical care if hives appear along with a tightening of the mouth or throat, swelling in the face, breathing problems, or fainting.
It is important to figure out the cause of hives. When they are triggered by a particular substance, avoiding that substance in the future can help prevent hives. Your doctor can help you determine if you are allergic to any foods, medications, or other substances, or are sensitive to another factor such as heat or sunlight.
What Causes Chronic Hives?
In about 80 to 90% of cases, doctors aren’t sure what caused chronic hives. They call these cases “idiopathic.” Some doctors think that idiopathic chronic hives may result from an autoimmune reaction in which the immune system attacks the body’s healthy tissue. One of the most common triggers of chronic hives is physical factors like pressure, water, vibration, or extreme temperatures. These factors may make hives appear or cause existing hives to get worse.
In some cases, chronic hives can be a signal of an underlying disease, such as an infection or thyroid disorder. For this reason, it is a good idea to talk to your physician if you are experiencing chronic hives. However, having an underlying disease is rare, and most cases of chronic hives are caused by some other factor.
Chronic Hives: Treatments
Generally, the first step in treating chronic hives is to use a type of medication called second-generation H1 antihistamines. These medications include:
- Claritin (loratadine)
- Clarinex (desloratadine)
- Zyrtec (cetirizine)
- Xyzal (levocetirizine)
- Allegra (fexofenadine)
If these medications don’t get chronic hives under control, doctors may recommend other strategies. This may include taking a higher dose of the same medication or trying other types of allergy medications. If these strategies are ineffective, people with chronic hives may be able to take immunosuppressive drugs (medications that calm down the immune system). Additionally, doctors may recommend steroid drugs for people with severe chronic hives.
Some complementary medicine approaches may also help. Chronic hives symptoms may come on less frequently and for shorter amounts of time when people undergo acupuncture treatments. Because stress can worsen hives, mental health therapies like hypnosis, relaxation exercises and other natural methods to boost one’s mood may also help treat chronic hives.
For a little over 1 in 3 people with chronic hives, symptoms disappear within a year. For others, symptoms may continue off and on for several years or for their entire life.
Rashes and Their Causes